Deadly Fungal Infection Spreading to New Parts of U.S., CDC Warns

While we’re months into the typical cold and flu (and COVID) season, additional threats have also been on the rise this winter. You’ve probably read about the measles outbreak, as well an uptick in Salmonella cases thanks to contaminated food. Along with those concerning developments, fungal infections are also making the rounds, including new cases of Candida auris (C. auris), which health officials warn can be deadly. Read on to find out where the Centers for Disease Control and Prevention (CDC) says C. auris is spreading, and how you can protect yourself.
RELATED: Dangerous Fungal Infection Spreading to New Parts of U.S., CDC Warns.
This fungus can be deadly for immunocompromised patients.
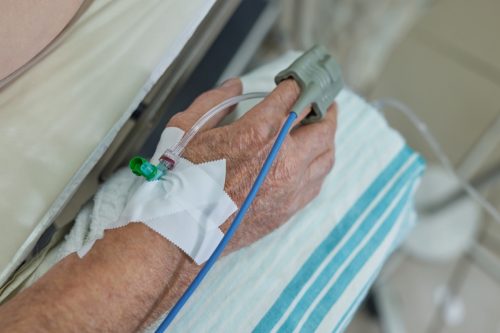
According to the CDC, C. auris is a type of yeast that spreads easily among patients at healthcare facilities, often causing severe illness. The agency notes that it is typically resistant to antifungal treatments, making it difficult to treat.
The fungus is particularly dangerous for people “with severe underlying medical conditions,” and those with “invasive medical devices like breathing tubes, feeding tubes, catheters in a vein, or urinary catheters tend to be at increased risk for getting C. auris and developing an infection,” the CDC says. Healthy people without these risk factors have a low risk of infection.
The severity of infection ranges from superficial skin infections to life-threatening ones, according to the CDC. However, as people who contract C. auris are often already sick, it’s difficult to know how big a role the fungus played in patients who have died.
Since 2016, the rate of C. auris infections has ticked up—and the CDC notes that cases “increased dramatically from 2020 to 2021.” Per a March 2023 press release from the CDC, the increase is likely due to “poor general infection prevention and control” at healthcare facilities, as well as an increase in screening.
RELATED: Salmonella Outbreak Spreading in 22 States—These Are the Symptoms.
C. auris established itself on the West Coast.

As of Dec. 31, 2022, the fungus was present in 36 U.S. states. Washington was one of the lucky states largely unaffected by the fungal infection, but now, officials in Seattle & King County confirmed the first outbreak at Kindred Hospital Seattle—First Hill, which is a long-term acute care hospital.
(The first locally acquired case in-state was reported last summer, per a July 2023 press release. The patient was a Pierce County resident who was transferred to Kindred, testing positive for C. auris on admission.)
On Jan. 22, two more patients treated at Kindred tested positive for C. auris. A fourth case with links to Kindred was reported on Jan. 26. As the public health department told NBC News, the fourth patient tested positive at a healthcare facility in Snohomish County, but had previously received care at Kindred.
Per Washington public health officials, all but one of the patients tested negative for the fungus when they were admitted to the hospital, suggesting that they picked it up on site. These patients were also isolated from the rest of the patient population “with extra clinical and cleaning precautions to prevent spread,” Kindred told NBC News.
Patients with C. auris were identified thanks to Kindred’s screening initiative, Partners for Patient Safety Program. The release from Seattle & King County notes that this was instated to increase early detection and prevent the spread of the fungus.
RELATED: COVID Now Causing These Unusual Symptoms, New Data Shows.
The spread is likely to continue.

In Washington, specifically, Peter Pappas, PhD, a professor of medicine at the University of Alabama at Birmingham, told NBC News that four cases of C. auris suggest that the fungus has been in the community for “quite some time.” However, experts don’t know how long that is.
According to Pappas, we shouldn’t expect C. auris to slow down, either.
“It will reach into every corner of the country for sure,” he told NBC News. “The question is going to be how well can we control it.”
Symptoms are inconsistent.
One Kindred patient developed an infection, health officials told NBC News, while others were merely “colonized” with C. auris. All were asymptomatic as of Jan. 31.
According to the CDC, colonization occurs when people get C. auris on their skin and other body sites but don’t get sick, show symptoms, or contract an infection. Even without symptoms, colonized patients can still spread the fungus to others or onto surfaces and objects that they come in contact with.
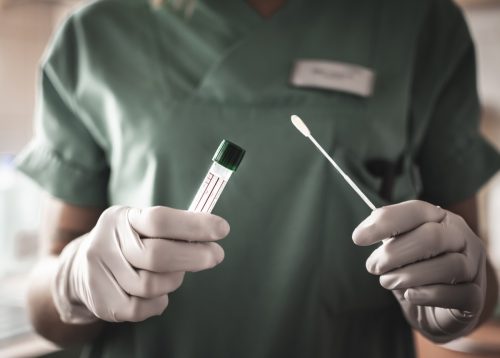
While healthy people don’t have to worry too much about C. auris, medical professionals stress the importance of screening. To screen for the fungus, healthcare professionals may swab the armpit or groin to collect a sample for testing. If symptoms show up that cannot be linked to anything else, a doctor may collect a blood or urine sample to screen for many types of infections. According to the CDC, there is no list of defined symptoms that can be used to identify C. auris.
“C. auris can cause infections in different parts of the body such as in the bloodstream, open wounds, and ears,” the CDC says. “The symptoms depend on the location and severity of C. auris infection. Symptoms may be similar to symptoms of an infection caused by bacteria.”
RELATED: For more up-to-date information, sign up for our daily newsletter.
Best Life offers the most up-to-date information from top experts, new research, and health agencies, but our content is not meant to be a substitute for professional guidance. When it comes to the medication you’re taking or any other health questions you have, always consult your healthcare provider directly.