21 Foot Symptoms That Indicate Bigger Health Problems

Occasional foot pain is fairly common—just ask anyone who’s spent the day wearing high-heeled shoes or who works a job that keeps them on their feet. But in some cases, consistent pain or discomfort in your feet or toenails can be a sign of an illness that needs to be addressed and treated by a doctor. Whether it’s flaky skin, numbness, swelling, or spider veins, here are 21 foot symptoms that reveal something you need to know about your overall health.
1
White, blue, or red toes: Raynaud’s disease

“If your toes turn white, then blue, and then go red, after which they return to their normal tone, it’s a symptom of Raynaud’s disease,” says practicing physician Nikola Djordjevic, MD. He explains that the color change is due to a sudden narrowing of the arteries, known as a vasospasm. Though it is sometimes hereditary, Raynaud’s disease “can be related to thyroid problems, rheumatoid arthritis, or Sjögren’s syndrome.” So if you notice this discoloration in your feet, consult your doctor to get to the bottom of it.
2
Round or clubbed toes and toenails: Lung disease

If you notice a change in the shape of your toenails (and fingernails) to the point that they are clubbed, Djordjevic warns you might have lung disease. And according to the doctor, these nails that are almost “half of a sphere” can also “be a sign of heart disease, digestive disorders, or liver problems.”
It’s important to note that clubbed toes are a symptom only if they are a result of change. If you have always had irregularly shaped toenails as a physical feature and they run in your family, there’s no need to be concerned.
3
Balding toes: Peripheral arterial disease

Losing some or all of the hair on your toes can be a sign of poor blood circulation caused by peripheral arterial disease. Also known as P.A.D., this disease occurs when narrowed blood vessels reduce blood flow to the limbs. Other P.A.D. foot symptoms include a weak or absent pulse in the foot and sores that don’t heal. Talk to your doctor if your toes suddenly become bald. The good news is that P.A.D. is treatable, typically through heart-healthy lifestyle changes, medication, and sometimes surgery.
4
Pain and tingling: Diabetes
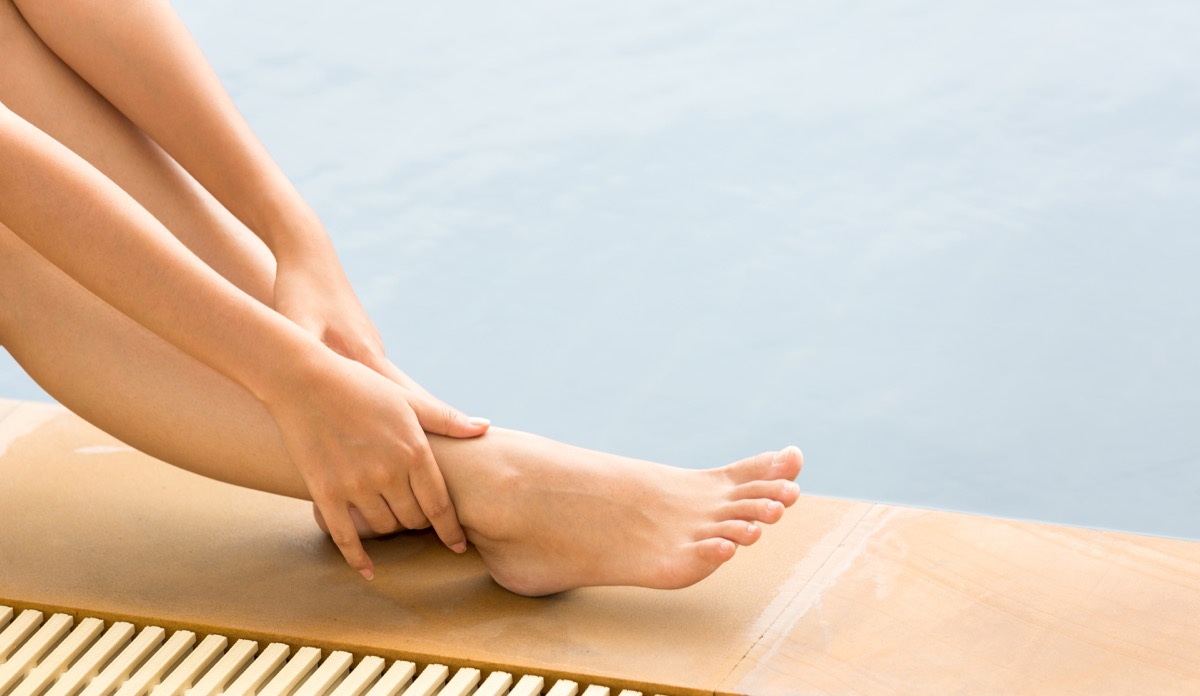
According to the National Institute of Diabetes and Digestive and Kidney Diseases, diabetes can cause nerve damage, known as diabetic neuropathy, in your feet, which in turn causes pain, numbness, and tingling sensations. If you experience these symptoms in your lower extremities, it could be a sign of this condition, and you should discuss it with your doctor.
5
Numbness and tingling: Multiple sclerosis (MS)
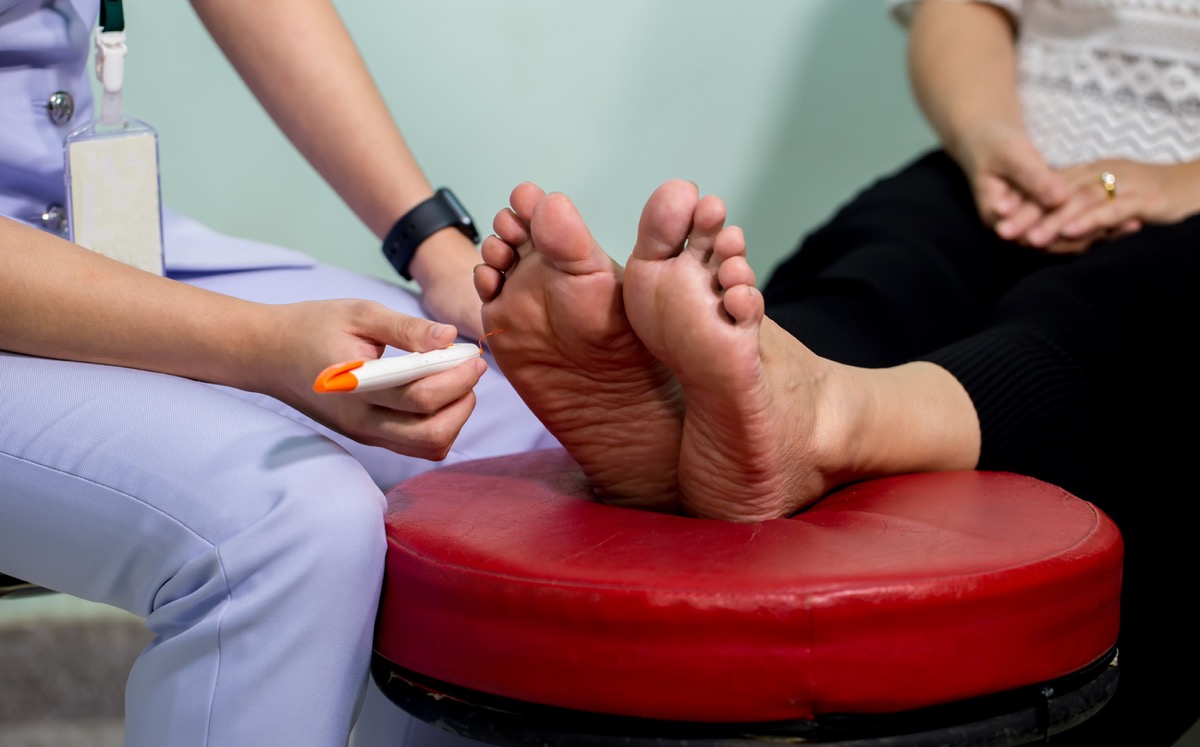
Numbness and tingling can also be a sign of multiple sclerosis, or MS. “One of the first symptoms of MS is often a numbness or tingling sensation, sometimes in your feet,” says Julie Fiol, RN, director of MS information and resources at the National MS Society.
In some cases, Fiol explains that one foot may have a different sensation than the other—for example, it might be more sensitive or you can’t feel it as well as you can your other foot. If you experience numbness or tingling in your foot, it’s important to inform your doctor immediately. MS is a serious illness that causes the immune system to eat away at the protective covering of nerves. It isn’t curable, but it is treatable with a doctor’s care and guidance.
6
Heel pain: Plantar fasciitis

Pain on the bottom of your foot in the heel area can be a symptom of plantar fasciitis, a common condition that occurs when the tissue supporting the arch of the foot becomes irritated and inflamed. But don’t worry too much about it: In the vast majority of cases, plantar fasciitis is easy to treat through rest and calf stretching exercises.
7
Pain and swelling: Gout

Scott Neville, DPM, a podiatrist in Mooresville, Indiana, says that for some people, pain and swelling in the foot can be a sign of gout.
“[Gout is] a type of painful inflammatory arthritis caused by too much uric acid in the blood,” Neville explains. “Tophi—which are uric acid crystal deposits that look like lumps under the skin—commonly develop [in the feet], although they can [also] be found in joints throughout the body.”
In many cases, gout can be managed by standard therapies and lifestyle changes. However, some people suffer from uncontrolled gout, which can cause long-term damage. Discuss your symptoms with your doctor to ensure you’re treating the condition correctly.
8
Restless feet at night: Iron deficiency

“Restless feet and legs at night is often a signal that you have an iron deficiency,” says Arielle Levitan, MD, a physician of internal medicine and co-founder of Vous Vitamin LLC. To help combat this symptom and the underlying issue, Levitan recommends taking a daily vitamin—and if even that doesn’t help, make sure to schedule an appointment with your physician.
9
Fungus between the toes: Athlete’s foot

According to Christopher Drumm, MD, a Pennsylvania-based primary care physician with Einstein Healthcare Network, if it looks like there’s fungus between your toes, you most likely have athlete’s foot. Other symptoms of athlete’s foot include a scaly rash, itching and burning, and blisters. Over-the-counter antifungal products usually do the trick, but if your symptoms don’t improve within two weeks, it’s time to see a doctor.
10
Not feeling pain when you should: Neuropathy
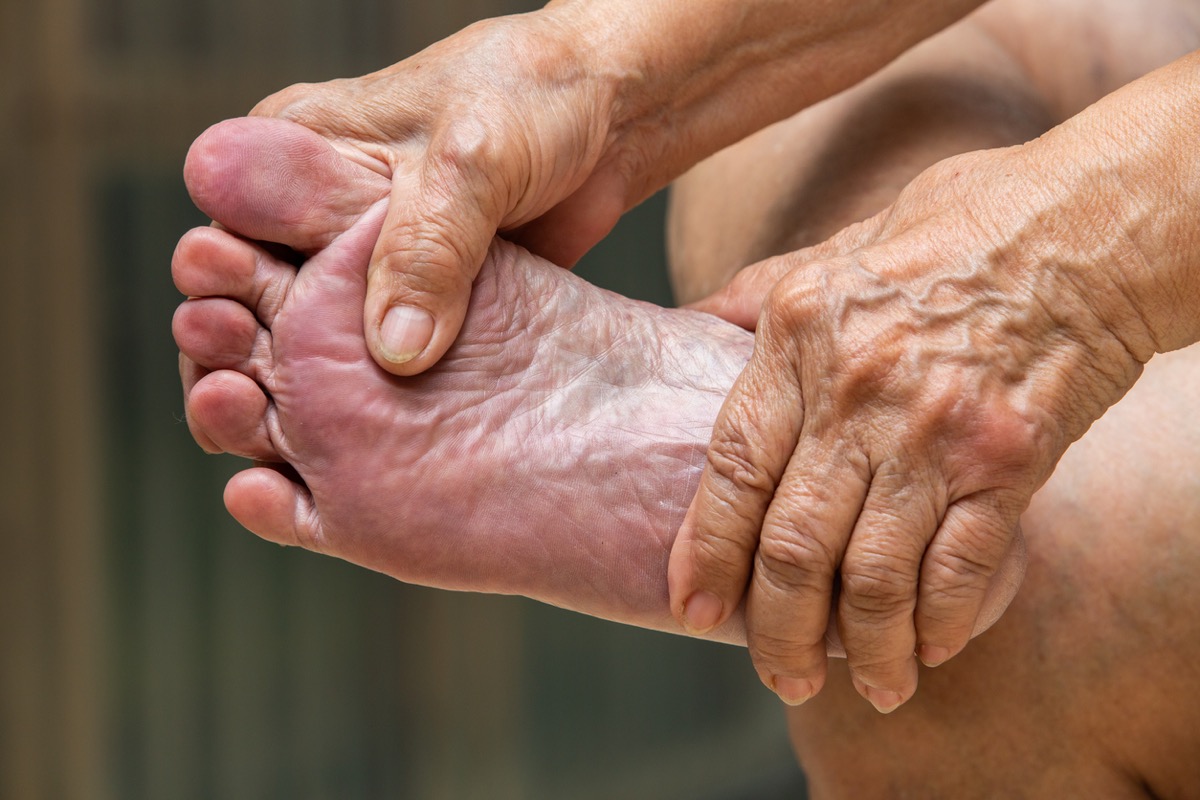
“If you step on a nail but don’t feel any pain, then you likely have neuropathy,” says Drumm. According to the Cleveland Clinic, anywhere from 25 to 30 percent of Americans and as many as 70 percent of people with diabetes are affected by neuropathy. However, that isn’t to say that this condition is harmless and should be left alone; neuropathy is the result of nerve damage, so you should see a doctor if you suspect you have the condition.
11
Spider veins and varicose veins: Venous reflux
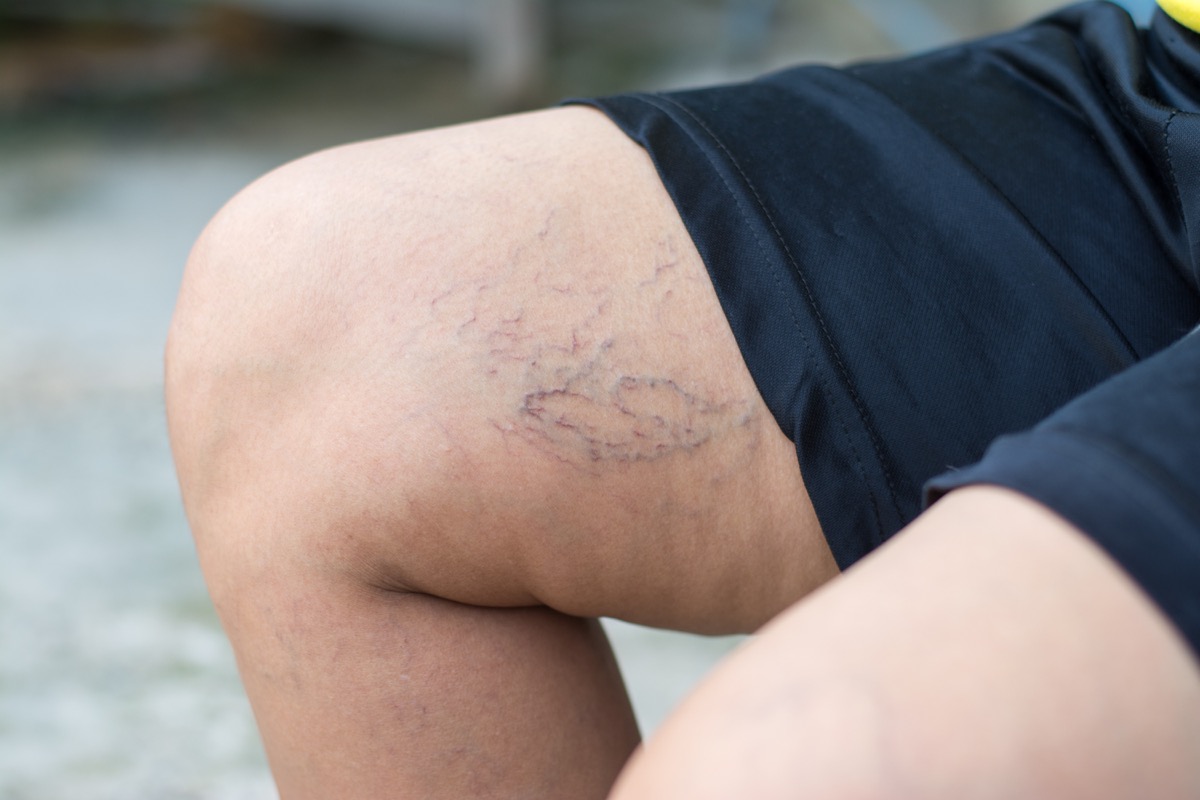
“Clusters of tiny blue and red blood vessels in the inner ankle may indicate an underlying problem [that’s] not visible to the naked eye,” says Nisha Bunke, MD, FACPh, RPhS, a vein specialist at La Jolla Vein Care in San Diego, California. She explains that these small veins are sometimes “the tip of the iceberg” and may be a sign of venous reflux, a condition that affects the circulation of blood in a person’s lower extremities.
If left untreated, venous reflux can lead to blood clots and hemorrhaging, so make sure to seek professional care if you have varicose pains coupled with any swelling or pain.
12
Darkening of the skin around the ankle: Chronic venous insufficiency
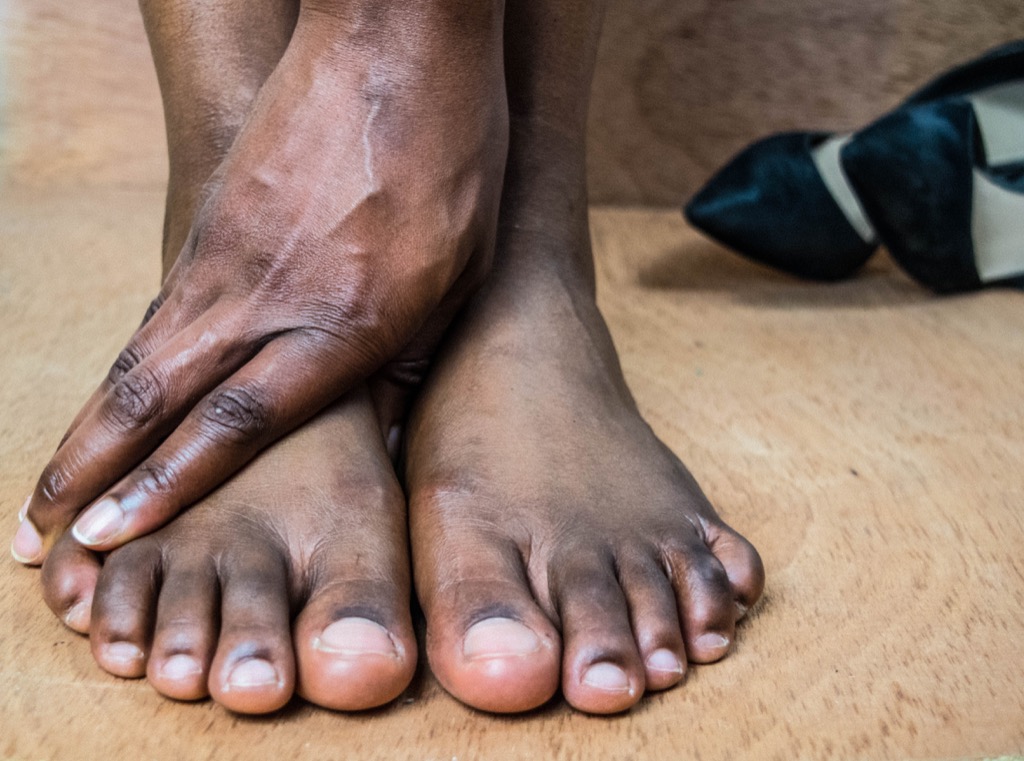
According to Bunke, the darkening of the skin around the ankle, also known as skin hyperpigmentation, is a sign of chronic venous insufficiency (CVI). This condition occurs when the valves in a person’s leg veins aren’t working effectively, causing blood to pool in the veins rather than return to the heart.
“This [symptom] usually occurs in the inner ankle and can worsen to involve the lower portion of the leg,” Bunke says. “Over time, the skin becomes firm, dry, eczema-like, and itchy and can even break open, causing a venous leg ulcer.”
13
Cold feet: Excess adrenaline

Michael E. Platt, MD, author of The Miracle of Bio-identical Hormones and Adrenaline Dominance, says that “the most common cause of cold feet is excess adrenaline, [which is] a survival hormone. Part of this response includes the cutoff of circulation to areas of the body not needed for survival.” Platt adds that cold feet (and hands) can also be caused by irritable bowel syndrome (IBS) and underactive thyroid. “However, this is rarely the case,” he explains.
14
Cracked heels: Underactive thyroid
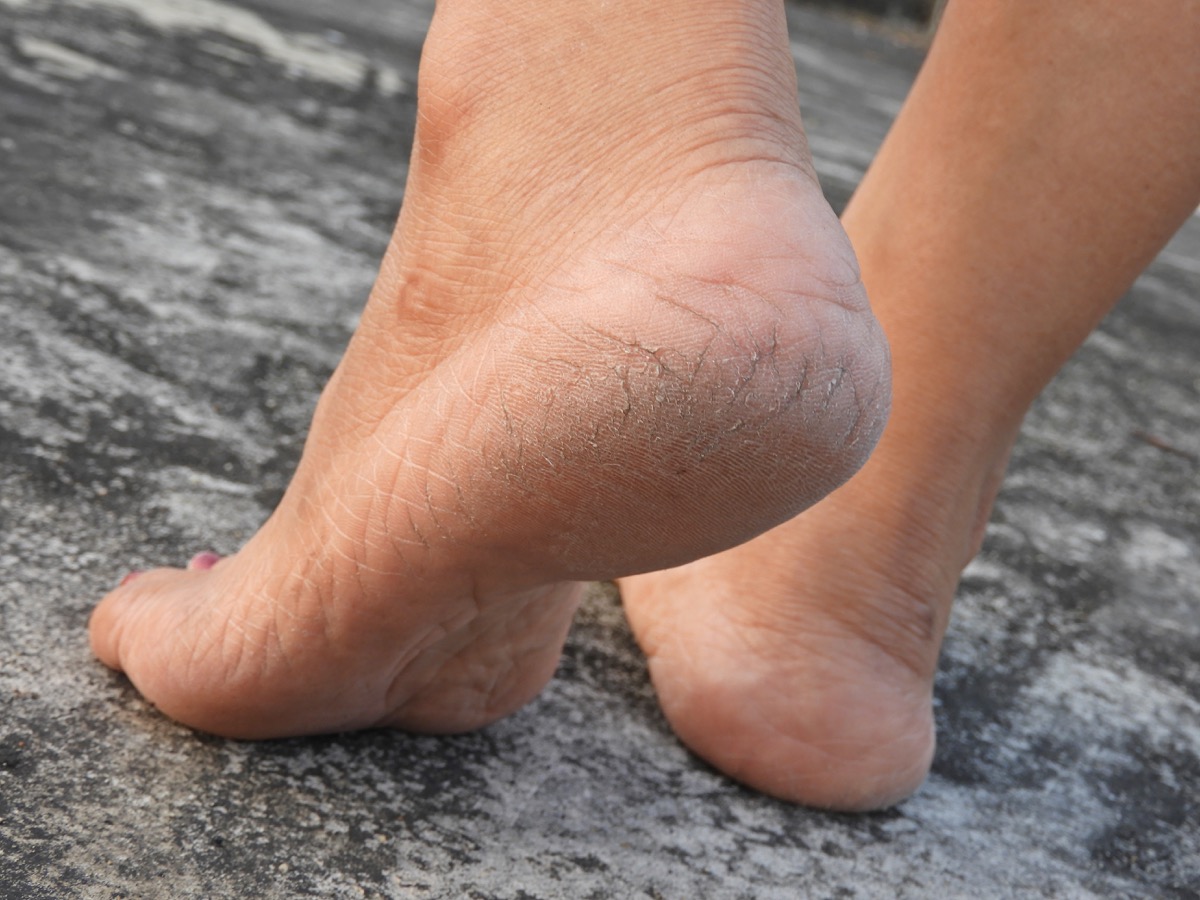
One foot symptom that is, however, linked to the health of your thyroid is cracked heels. “Skin that is cracked over the heels is a classic sign of an underactive thyroid,” Platt says. Other symptoms include weight gain, depression, muscle aches, and fatigue.
15
Pain and stiffness: Arthritis

Although we don’t typically associate arthritis with the feet, the autoimmune illness can cause pain and stiffness in both the foot and ankle, according to the American Academy of Orthopaedic Surgeons. Though there are more than 100 forms of arthritis, the ones most likely to cause foot and ankle pain are osteoarthritis, rheumatoid arthritis, and posttraumatic arthritis.
Arthritis might be a common age-related condition, but it’s also treatable, so talk to your doctor if you’re experiencing stiffness.
16
Pitted toenails: Psoriatic arthritis

According to the National Psoriasis Foundation, pitted toenails—that is to say, toenails with indentations or depressions in them—can be a symptom of psoriatic arthritis. Other symptoms include changes to the nail’s shape, discoloration of the nail, thickening of the nail, and onycholysis, or the separating of the nail from the nail bed. It’s important to note that these are also symptoms of nail psoriasis, so you should visit a doctor to get an exact diagnosis and treatment plan.
17
Green toenail: Chloronychia
If you notice that your toenails are turning green, it may be due to chloronychia (also known as green nail syndrome). Chloronychia is caused by the bacterium Pseudomonas aeruginosa, and it often presents itself after the foot has had prolonged exposure to water or certain soaps and detergents.
On the bright side, treatment is relatively simple: It usually involves a lot of medical soaking and keeping the nails otherwise dry.
18
Swollen ankles: High blood pressure

High blood pressure forces your heart to work overtime, and this effort can cause the muscle to thereby become less effective at circulating your blood. As a result, fluid builds up in the lower legs and ankles, causing them to become swollen. So don’t write off that swelling as foot-specific—see a doctor to get it checked out before things become even more dire.
19
A black or brown streak under the toenail: Subungual melanoma
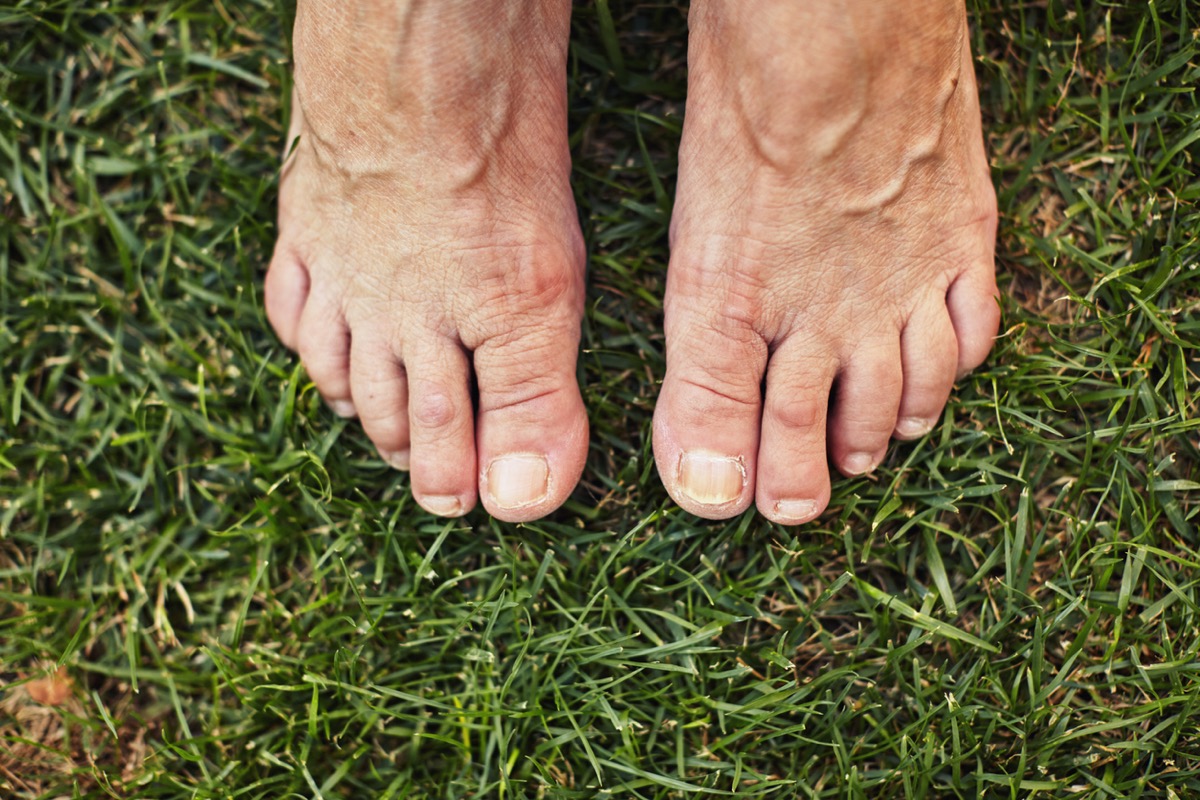
A black or brown streak under your toenail might look like a mere bruise (and sometimes it is), but it can also be a sign of subungual melanoma, a form of skin cancer. If this streak doesn’t heal or if it increases in size, make an appointment with your dermatologist as soon as possible.
20
Thick, yellow toenails: A fungal infection

A thick, yellow toenail is usually a sign of a fungal nail infection, according to the Centers for Disease Control and Prevention (CDC). Though the infection usually isn’t painful unless it becomes severe, it’s notoriously difficult to treat. When you visit the doctor for treatment, they will likely prescribe oral antifungal pills—though if they’re ineffective and the case is severe, your toenail may need to be removed completely.
21
Difficulty lifting the front part of the foot: Charcot-Marie-Tooth disease

Trouble lifting the front part of your foot (also known as a foot drop) can be a sign of Charcot-Marie-Tooth disease (CMT), according to the National Institute of Neurological Disorders and Stroke. Other common symptoms of CMT include trouble walking and sudden foot deformities like high arches and hammertoes.
If you’re worried that you are dealing with CMT, seek the opinion of a medical professional. Though there isn’t a cure for CMT, it can be treated with physical therapy, occupational therapy, and orthopedic devices. And for more signs to look out for for an overall healthier you, check out these 23 Subtle Signs of Serious Health Issues.
To discover more amazing secrets about living your best life, click here to follow us on Instagram!