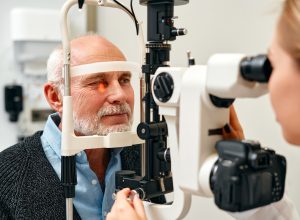
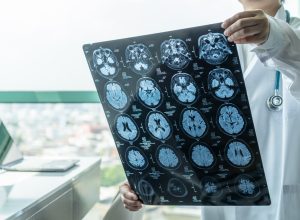
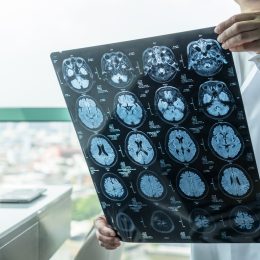
How Your Nose Can Predict Alzheimer's
It could pick up on the disease years earlier.
4 Vaccines That Can Lower Your Risk of Dementia
If you're over age 65, this is an important read.
Common Vaccine Can Lower Your Risk of Dementia
It could also help with heart attack and stroke.
The No. 1 Beverage to Protect Your Brain After 60
Coffee drinkers, take note.
Common Virus Could Increase Alzheimer's Risk By 80%
Researchers have found a shocking new connection.
Do Anxiety Meds Raise Dementia Risk?
The science just flipped.
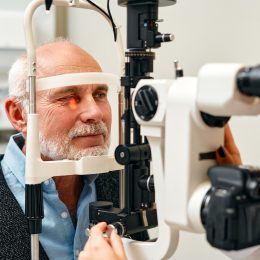
Your Annual Eye Exam Could Detect Alzheimer's
Your retinas have identical tissue to your brain.
2 Supplements Can Slow Down Alzheimer’s Disease
New research shows the benefit of taking them together.
Superfood Can Lower Dementia and Alzheimer's Risk
Skipping it is linked to a fourfold increase in dementia risk.
This Supplement Could Protect Against Dementia
Adults 75+ have trouble absorbing the vitamin from food.
Common Diabetes Drug Can Protect Against Dementia
The common med can also prevent Alzheimer's, research shows.
"Super-Agers" Have These 4 Things in Common
At age 80, they remember nearly everything.
5 Symptoms That Can Predict Multiple Sclerosis
Doctors say it can detect MS up to 15 years sooner.
"Dirt Cheap" Treatment Could Reverse Alzheimer’s Disease
Scientists discover a new use for lithium.
5 "Healthy" Habits Silently Harming Your Brain
These can raise your risk of cognitive decline.
4 Simple Lifestyle Changes Can Reduce Your Dementia Risk
A new study promotes these changes over age 60.
It Can Take 4 Years to Diagnose Dementia, Research Shows
10 Early Signs to Look Out For
4 Ways Your Gut Health Is Affecting Your Brain
Doctors say these issues start in your GI tract.
This Essential Mineral Could Protect Your Brain
It's especially helpful if you're over 60.
Eating This Food Reduces Alzheimer's Risk
Just two servings a week cuts it by 47%.