Leprosy Cases Are Rising in the U.S.—These Are the Symptoms to Know
From the human plague to measles and mumps, we’ve recently seen a resurgence of several uncommon sicknesses. But now, disease specialists are also warning that leprosy is making its way back, according to a new report from Newsweek. Clinically known as Hansen’s disease, leprosy is very rare in the U.S. However, the Centers for Disease Control and Prevention (CDC) released a report this past summer warning that leprosy cases in the country have started increasing during the last decade.
The National Hansen’s Disease Program (HRSA) indicates that a record 216 new cases were reported nationwide in 2019. This fell to 159 in 2020 and 124 in 2021 but started rising again in 2022 with 136 new cases. National data for last year has not been officially released yet.
Most of the new leprosy cases have been found in seven states: Florida, Texas, New York, California, Arkansas, Louisiana, and Hawaii. But the real concern is in just one of these states.
“Florida reported 10 cases of leprosy every year between 2002 and 2014. This rose to 29 new cases in 2015. There were 15 new cases in 2023,” Francisca Mutapi, professor in Global Health Infection and Immunity and co-director of the Global Health Academy at the University of Edinburgh, told Newsweek.
Leprosy is an infection caused by the Mycobacterium leprae bacteria, and it is believed that prolonged close contact with an infected person can spread the disease. In the southern U.S., armadillos naturally infected with this bacteria may be able to spread it to people, according to the CDC. But the agency says, “Most people with Hansen’s disease in the U.S. became infected in a country where it is more common.”
However, the CDC noted that Florida’s “increased incidence of leprosy cases” has lacked traditional risk factors, mainly that 34 percent of the new case patients in this state from 2015 to 2020 “appeared to have locally acquired the disease,” indicating that leprosy has likely become endemic in the southeastern U.S.
While leprosy is no longer feared to be a highly contagious disease, it can cause nerve damage, paralysis, and blindness if left untreated. So it’s important to know what you should be looking out for. Read on to learn about the most common leprosy symptoms.
RELATED: Norovirus Cases Spiking Across U.S.—These Are the Symptoms.
1
Discolored patches of skin
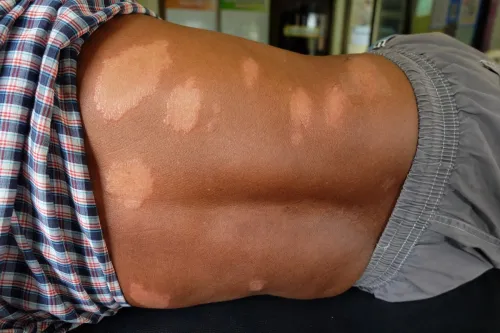
Leprosy is most known for its impact on the skin. It can be recognized by the appearance of discolored “patches of skin that may look lighter or darker than the normal skin,” according to the CDC. The agency says the affected skin areas may also appear reddish.
2
Lumps and ulcers
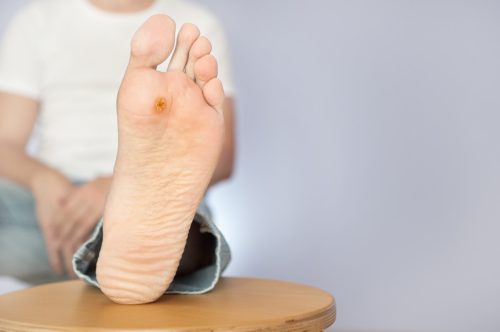
Aside from discolored patches, leprosy can also cause growths on or under the skin. This may include “painless ulcers on the soles of feet” or “painless swelling or lumps on the face or earlobes,” according to the CDC.
3
Loss of eyebrows or eyelashes

Hair loss is another possible symptom of leprosy. Specifically, the CDC says you may experience the loss of eyebrows or eyelashes with this disease.
RELATED: Ulcer-Causing Skin Infection From Tropical Parasite Now Spreading in U.S., CDC Warns.
4
Stuffy nose and nosebleeds

Leprosy can also affect mucous membranes in the lining of the nose. As a result, you may experience a stuffy nose and/or nosebleeds as symptoms.
5
Numbness

The bacteria behind leprosy can attack nerves, which may lead to numbness in the affected areas of the skin.
“Since Hansen’s disease affects the nerves, loss of feeling or sensation can occur. When loss of sensation occurs, injuries such as burns may go unnoticed,” the CDC explains.
Best Life offers the most up-to-date information from top experts, new research, and health agencies, but our content is not meant to be a substitute for professional guidance. When it comes to the medication you’re taking or any other health questions you have, always consult your healthcare provider directly.
- Source: CDC: Case Report of Leprosy in Central Florida, USA, 2022
- Source: HRSA: National Hansen's Disease (Leprosy) Program Caring and Curing Since 1894
- Source: CDC: Hansen's Disease (Leprosy)
- Source: CDC: Hansen's Disease Transmission
- Source: CDC: Leprosy Diagnosis and Treatment
- Source: CDC: Leprosy Signs & Symptoms